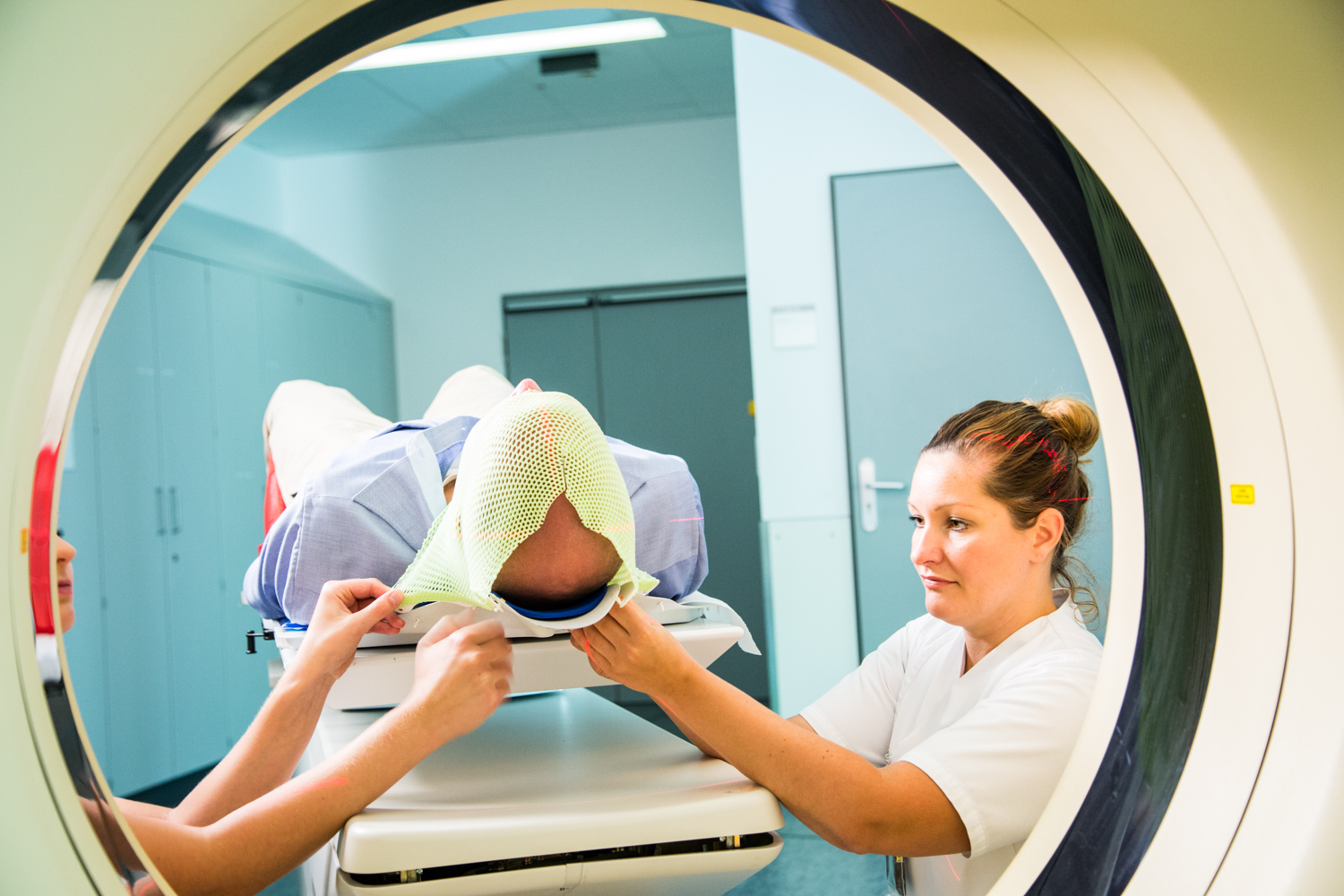
Treatment procedure
Proton therapy at WPE takes place on an outpatient basis. For better tolerability, the required radiation dose is spread over several weeks. Five days a week for a period of six to eight weeks, you will come to the WPE on a daily basis.
The treatment takes about 30 minutes on average, including the positioning aids. The actual irradiation takes only a few minutes.
In our video we give you a short insight into the treatment process of proton therapy at WPE.
Our radio-oncologist accompanies the proton therapy at the WPE. According to the particular disease, an inter-disciplinary collaboration with the other specialist clinics of the University Hospital Essen is meaningful. All children are therefore also cared for by the paediatric oncologists of the University Hospital Essen. Don’t forget to bring personal documentation or medication if you are not coming from the immediate vicinity of Essen. You will spend several weeks in Essen.
After-care
Your therapy always concludes with a final examination. Three months later the first post-therapeutic examination takes place. Thereafter an annual follow-up examination takes place over a period of five years. The regular follow-up controls are fundamentally planned at the WPE, but are also determined in consultation with the doctors at home.
We also document the results of the follow-up controls in our studies in order to enable long-term prognoses. You’ll find information about voluntary participation in the respective studies here and also during the discussions relating to the initial presentation. In the event that your follow-up controls are not performed at the WPE, a questionnaire will be sent to you and your attending doctor in order to gather your data.
We shall invite you to the regular follow-up sessions.
Possible side effects
Radiotherapy is a local measure. In the event that a reaction occurs, usually only the irradiated region of the body is affected. This can be in the form of irritations of the skin or mucous membranes – these usually vanish completely two or three weeks after irradiation. However, permanent scarring may occur as a long-term effect.
In general, fatigue, listlessness or lack of appetite can also occur with patients as a result of the body’s stress in the face of coping with the radiation. However, the possible side effects described depend upon the irradiated region and the radiation dose and are discussed in detail in the information session.
Contact us
The case management of WPE will assist you with questions you may have.
Phone: 0201 723 6600
