Proton Therapy
characteristics and impact
General information on radiotherapy: the aims, the benefits and the right dosage
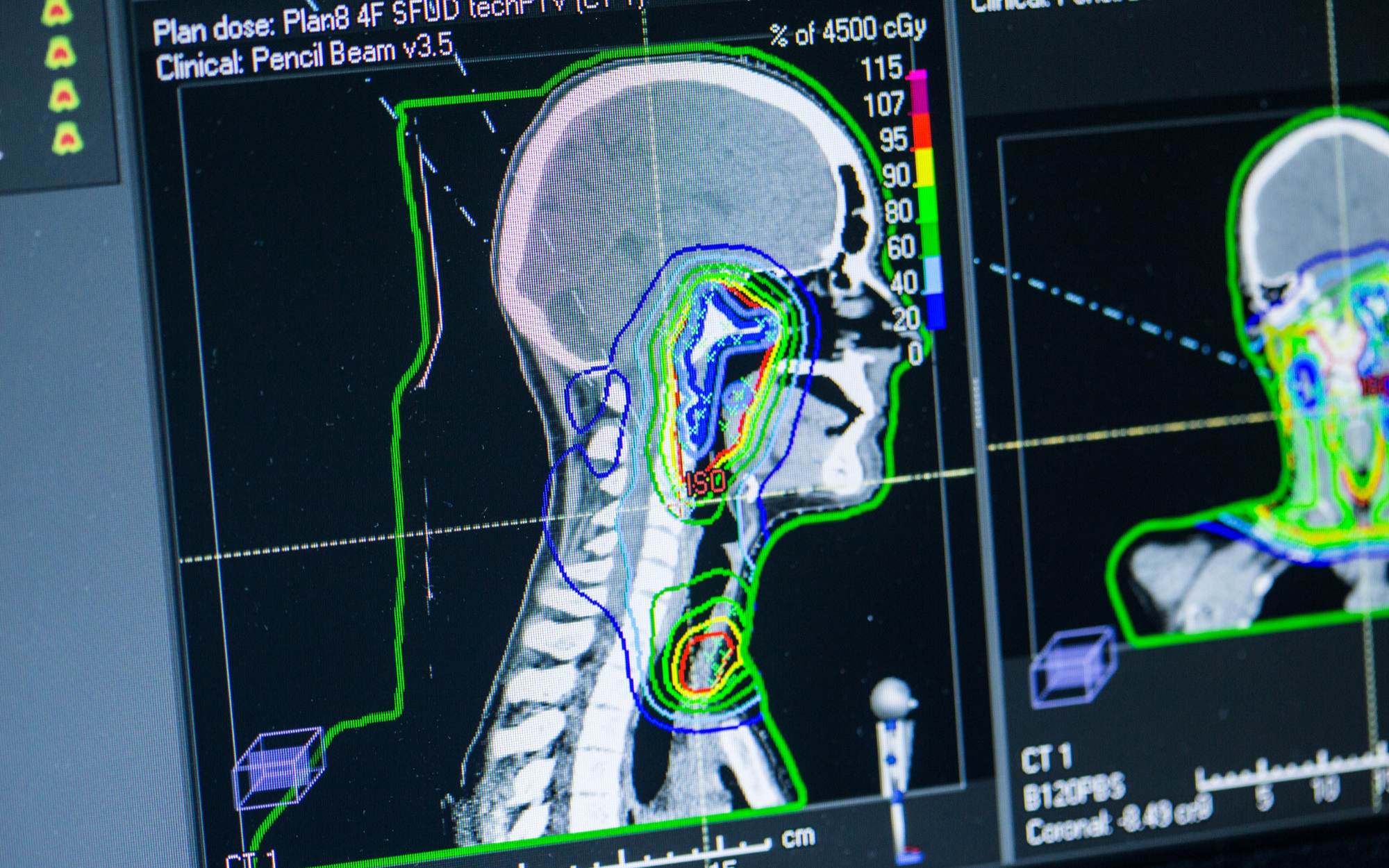
The aim of radiotherapy is always to destroy the DNA in the tumour cells in order to stop their ability to divide and thus grow. To do this, energy packets or particles are brought to a very high energy level in so-called accelerators so that they can penetrate the diseased tissue and do their work there. The advantage of radiotherapy is that it is localised and thus only affects a specific, defined area of the body: in the tumour itself. This reduces side effects and distinguishes radiotherapy from chemotherapy, which has a different (‘systemic’) mode of action, acting throughout the human body. Spreading the radiotherapy dose over several radiotherapy sessions reduces the side effects even further, making radiotherapy more tolerable for the patient.
Different tumours require different dosages
During radiotherapy, energy packets or particles are brought to a very high energy level in so-called accelerators so that they can penetrate the tissue and do their work there. The absorbed dose is measured in ‘Grays’ (abbrev.: Gy), which is the unit of measure indicating the dosage of radiation treatment. In radiotherapy, some tumours can be impaired by a low dose of radiation, whereas other tumours require a very high dose. This means that different tumours have different levels of sensitivity to radiation, therefore requiring different radiation dosages depending on the type of tumour involved.
Contact us
The case management of WPE will assist you with questions you may have.
Phone: 0201 723 6600
What is proton therapy?
Proton therapy, also referred to as proton treatment, is a modern form of radiotherapy for treating tumours in cancer patients. Its physical properties mean it can offer various benefits compared to photon-based radiotherapy:
- It is extremely precise as the protons can be aimed at the diseased tissue with millimetre precision.
- It can therefore mean fewer side effects.
- It ensures efficient tumour treatment as the surrounding healthy tissue is spared as much as possible.
Photon-based radiotherapy has been used for decades in treating tumours across the world. There are currently five facilities in Germany, of which WPE at the University Medical Centre of Essen is the largest. Its expertise in the field of research and its wide range of proton therapy applications – such as pencil beam scanning – have helped make WPE a highly respected treatment centre and a leader in proton irradiation.
Years of experience in proton therapy
The first research into proton therapy was carried out in the 1940s. The first purely medical proton therapy centre opened in the USA in 1991, and since then almost 300,000 treatments have been conducted worldwide.
Mode of action and the benefits of proton therapy
Proton therapy differs from conventional photon-based radiotherapy in many respects:
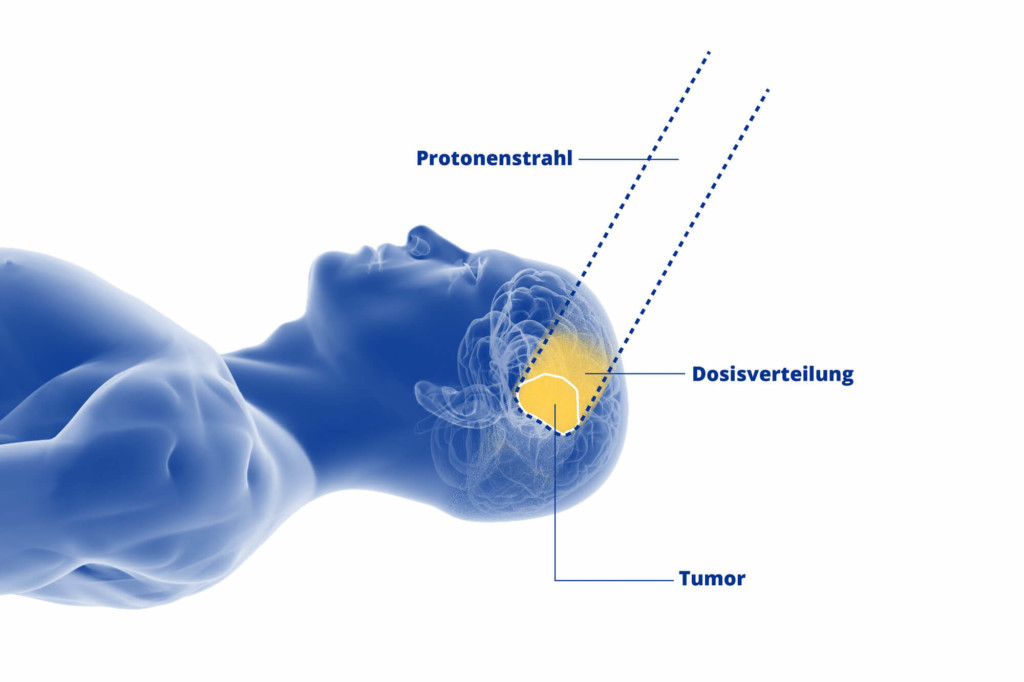
Proton-based treatment offers the key benefit of having only minor effect on healthy tissue. The reason for this lies in the focused proton beam which emits very little energy on its way to the diseased tumour cells. Most of the energy is discharged directly at the intended location – within the tumour itself.
As soon as the beam reaches the tumour, it stops abruptly (Bragg peak), meaning that the healthy tissue surrounding the tumour is exposed to significantly less radiation – both before and behind the tumour.
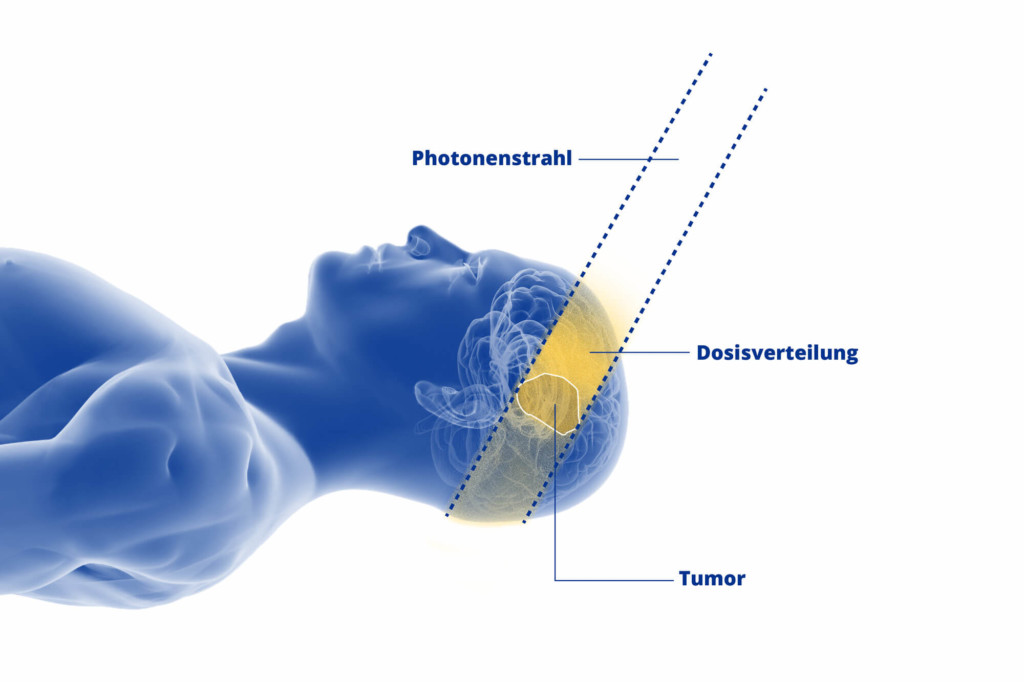
In radiotherapy using photons, the energy is emitted immediately it enters the body, meaning that healthy tissue receives comparatively more radiation. Neither can photons be stopped immediately after passing through the tumour.
Since tumours can be located at different depths in the body, the proton beam must be adjusted precisely to this depth. This is done via the speed. The deeper a tumour is located, the higher the speed of the proton beam must be.
This means the penetration depth of the protons can be adjusted precisely and the proton beam can be adapted precisely and individually to suit the shape and position of the tumour. For maximum efficiency in cancer treatment.
To enable this to be calculated, a team of case doctors and physicists always localises the exact position of your tumour before the actual proton therapy commences. This is done using CT and MRI images created specially for each patient.
With the help of these images, it is possible to determine the exact proton speed required for successful irradiation. This means the penetration depth of the protons can be adjusted precisely and the proton beam can be adapted precisely and individually to suit the shape and position of the tumour. For maximum efficiency in cancer treatment.
In clinical operation, protons can also be superimposed with different energies (stopping at different Bragg peaks). This means that even an extensive tumour can be irradiated evenly and with millimetre precision – for maximum protection of surrounding tissue and the best possible therapeutic outcome.
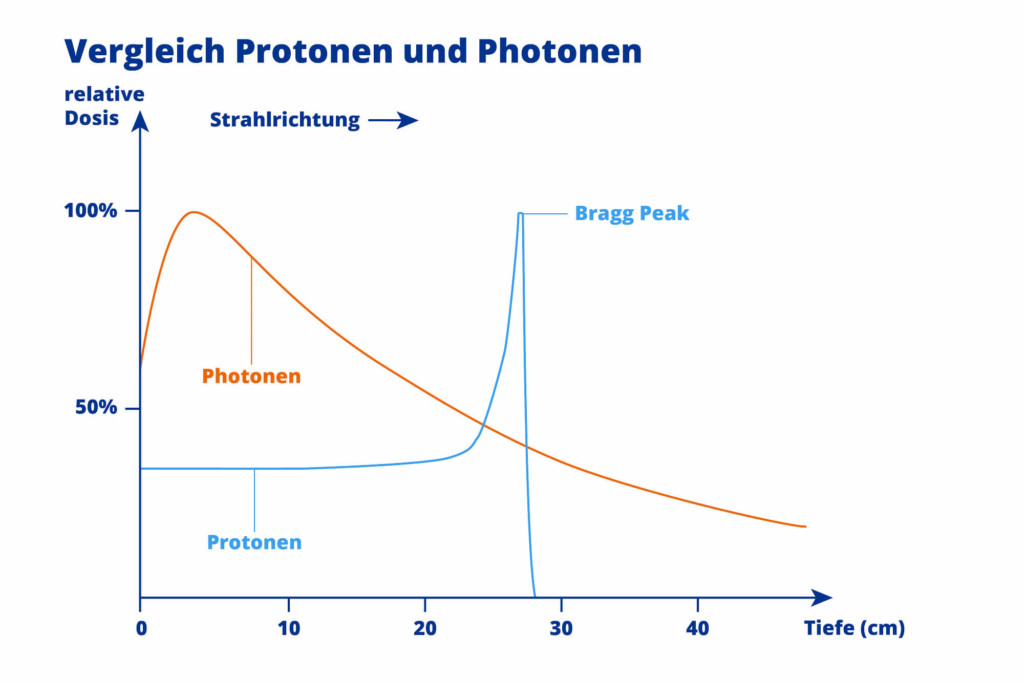
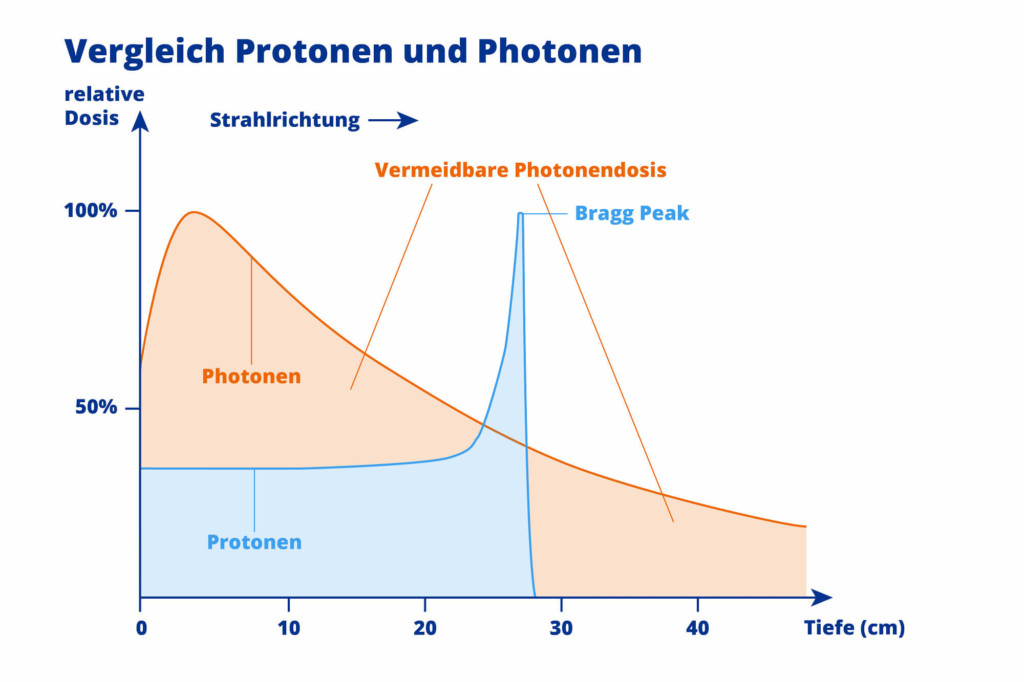
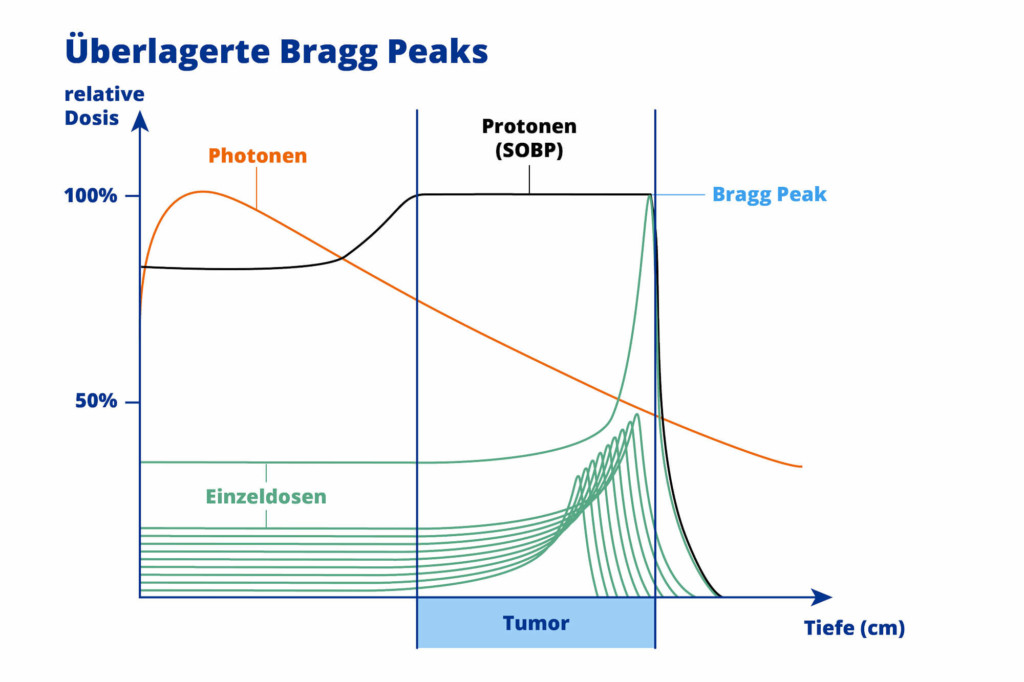
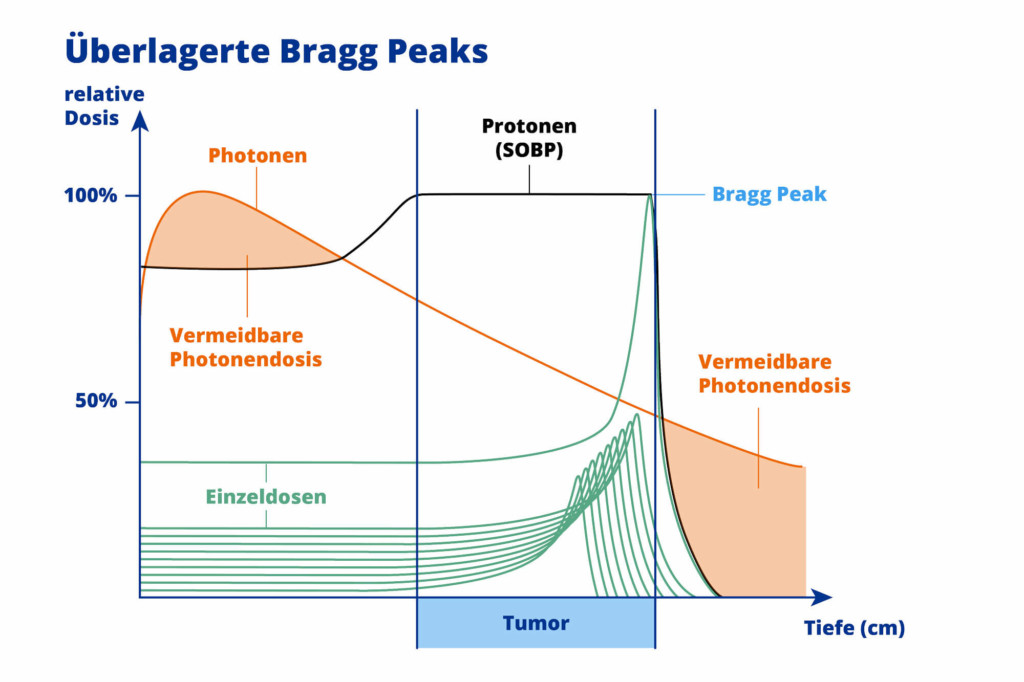
In contrast to conventional radiotherapy using photons, protons can penetrate much deeper into human tissue. Up to 30 cm deep. This means that proton therapy can also be used to irradiate deep-seated tumours effectively and with few side effects.
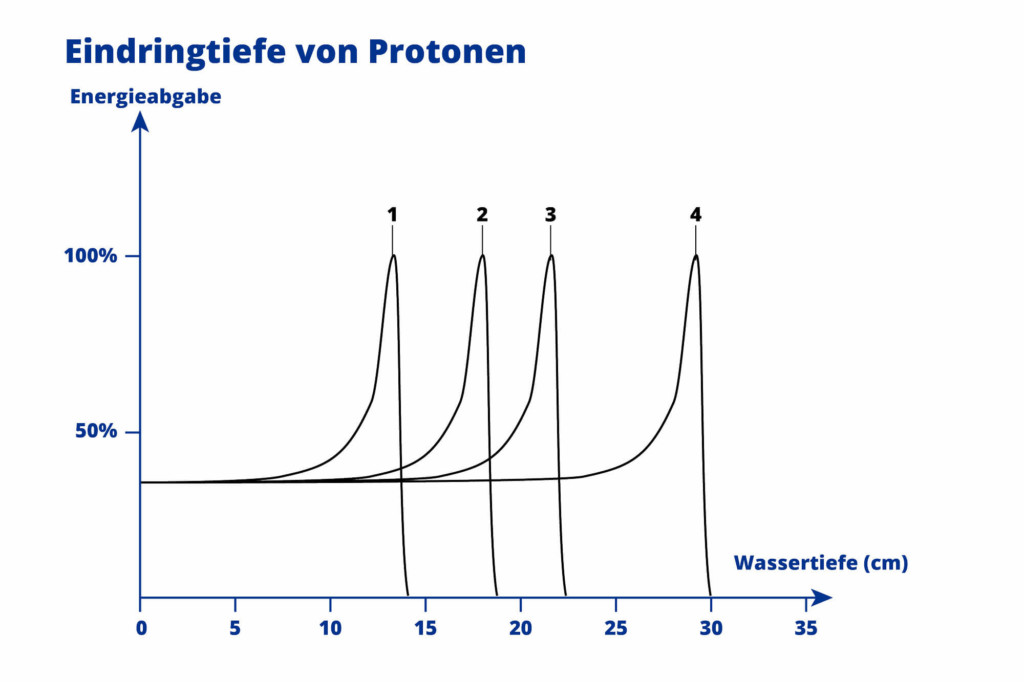
Especially for children with cancer, it is important to protect healthy tissue as much as possible during radiotherapy. Because children are still growing, irradiating healthy organs can have far-reaching consequences:
- Circulatory disorders
- Mutations in the central nervous system
- Growth and metabolic disorders
- Deterioration of hearing and vision
- Dental, orthodontic and mouth disorders
- Secondary tumours
- etc.
With proton therapy, disadvantages in the form of such late complications and long-term consequences are reduced to a minimum. This is because the lower energy output in front of the tumour and precise control of the proton speed make it possible to irradiate the child’s tumour as precisely as possible – for efficient, gentle treatment offering the best possible chances of recovery. This gentle treatment also makes the child’s time during radiotherapy easier, as acute side effects are also minimised. However, even with proton therapy not all side effects can always be avoided. In certain constellations, a balance may have to be struck.
Proton therapy for childhood cancers
If you would like to find out more about proton radiotherapy for children, read our article on proton therapy for children with cancer.
Where do the protons used in proton therapy come from?
Proton irradiation is a medical treatment using a complex physical process that begins simply enough: with a gas cylinder. This gas cylinder contains hydrogen which is split into its hydrogen atoms using a specific process, creating what are known as positively charged particles – protons.
Protons have the benefit that they can be directed very effectively with the aid of magnets. This makes it possible to accelerate them up to 180,000 kilometres per second in a cyclotron, a ring accelerator weighing over 200 tonnes and consisting of two gigantic magnetic discs. That’s around 60% of the speed of light.
This high speed ensures that the proton beam penetrates deep into the body, where it does its good work in treating the tumour. The patient is shown into one of our four treatment rooms. There, the beam head is adjusted with millimetre precision and controlled very specifically to irradiate the tumour with pinpoint accuracy. Three of the four radiotherapy treatment rooms also have so-called gantries which can rotate the beam through 360 degrees around the treatment table.
The proton therapy technique at WPE
The following video explains the technology behind proton therapy. Watch the video now and learn more.
Which diseases can be treated using proton therapy?
To date, almost 300,000 patients across the world have been treated successfully using protons. With technical progress and increasing investment, proton therapy is becoming more and more widely available, and the number of indications – i.e. the medical conditions for which it represents a viable alternative therapy – are also increasing steadily.
Very good results have been achieved with proton therapy, particularly on deep-seated tumours and on tumours surrounded by important or sensitive parts of the body. These include primarily tumours in the head, spinal column and pelvic area (i.e. mainly primary brain tumours) as well as sarcomas of the base of the skull, facial bones, spinal column and pelvis.
A standard indication for proton therapy is the treatment of uveal melanomas. Prostate and nasopharyngeal carcinomas are also suitable for treatment with proton therapy. In both cases, patients benefit from the precision of proton radiotherapy, as the bladder and bowel as well as the optic and auditory nerves can be spared as far as possible.
The same goes for the pituitary gland which is important for the production of hormones throughout life. It can be spared to best effect when proton therapy is applied to the head. As young tissue in children is particularly sensitive during the physical development stage, young patients – and in some cases very young patients – are an extremely important demographic when it comes to proton therapy. Here, proton therapy can be used to achieve the best possible avoidance of late complications and side effects.
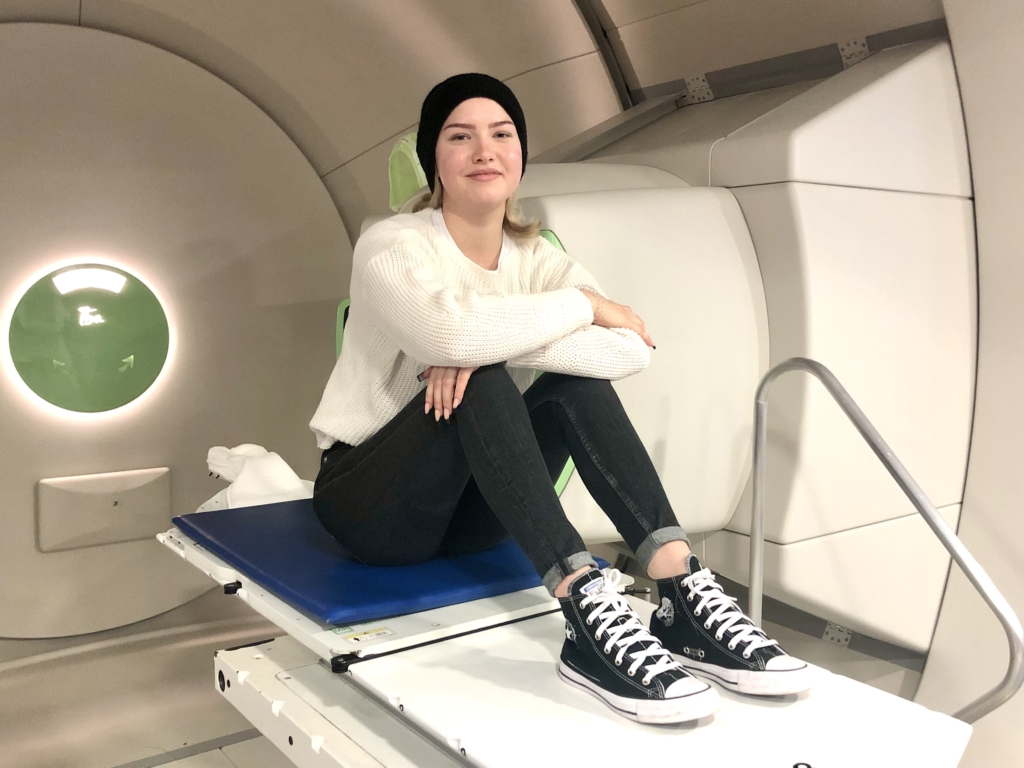
The pediatric oncology radiotherapy program at the WPE is the largest of its kind in Germany
2000 children have been treated at the WPE since the center opened in 2013. They…
Tumours treatable at WPE, the West German Proton Therapy Centre Essen
If you want to find out which tumours can be treated at WPE using gentle proton therapy, the article below will supply all the information you need.
Proton therapy and side effects
Radiotherapy is always accompanied by certain side effects. Depending on the area being treated, this can include nausea and vomiting, and also tiredness, fever and hair loss. Late complications such as secondary tumours can also occur. It is therefore all the more important to reduce these side effects to an absolute minimum, and to this end – depending on the indication – proton therapy is usually the treatment of choice. Patients generally tolerate proton treatment well. As far as the tumour itself permits, as a patient you can usually go about your everyday life without too many side effects. That said, acute side effects can occur, for example if you are taking additional medication or receiving chemotherapy. In any case, always talk to your case doctor if you experience any side effects during treatment.
More about proton therapy and side effects
If you want to find out more about proton therapy and its potential side effects, the following article will tell you all you need to know.
Contact us
If you would like more information on proton therapy, please contact us.
All initial contact is handled by our experienced, dedicated Case Management unit – the interface between you and our team. If you come to us for treatment, Case Management will also be happy to help you compile your documents, arrange cost coverage and make travel or accommodation arrangements, and will be happy to answer any questions you may have. Case Management will also put you in contact with our radiotherapists. Feel free to make your enquiries in English or in German.
Case management
The case management of WPE will assist you with questions you may have
Phone: 0201 723 6600