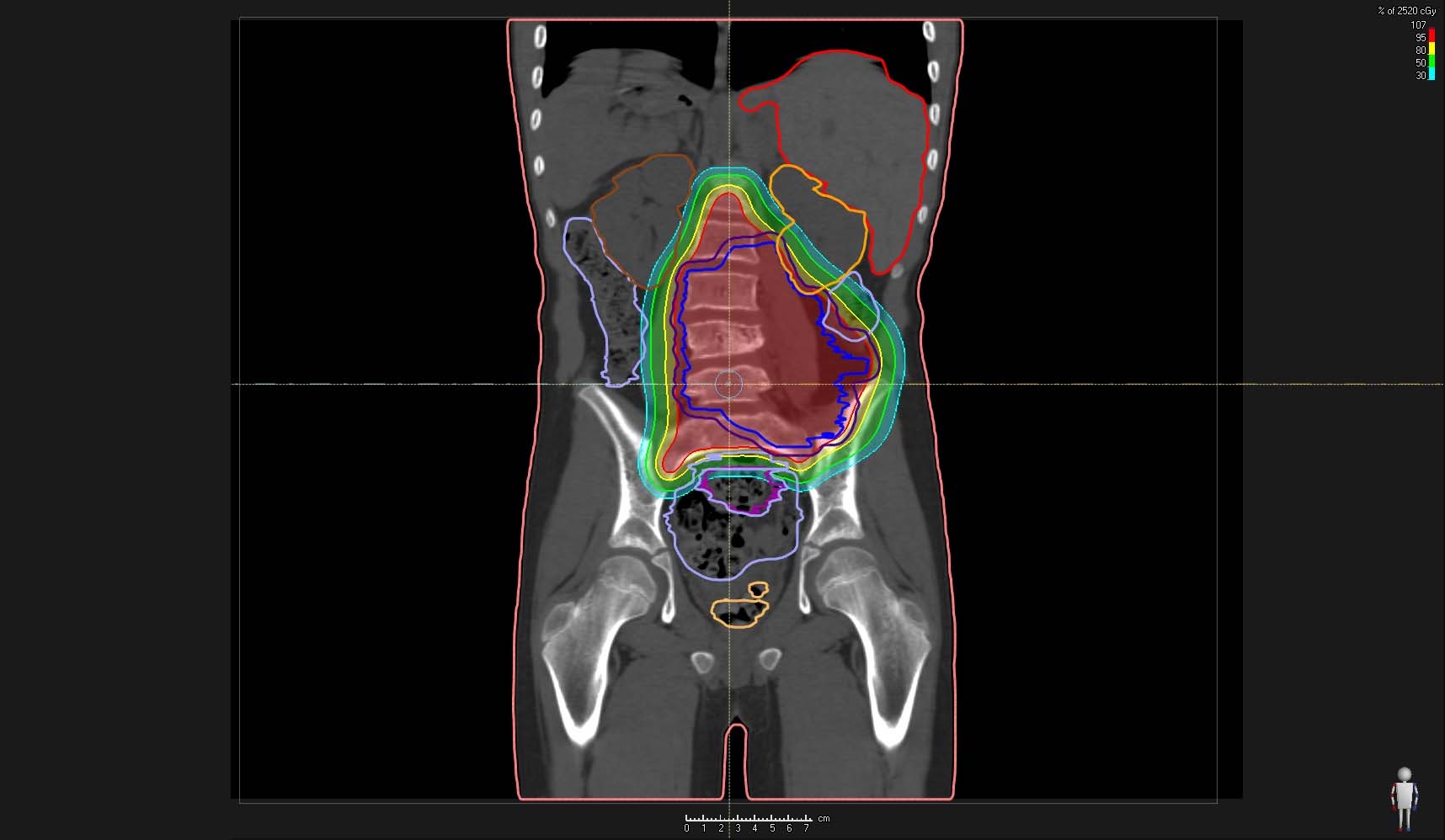
Proton therapy
for sarcomas
at WPE
Everything you need to know.
Definition, development and frequency of sarcomas
What are sarcomas?
Sarcomas are malignant tumours that can occur almost anywhere in the human body. They are roughly divided into two different groups:
- Soft tissue sarcomas (approx. 85% of cases)
- Bone sarcomas (approx. 15% of cases)
Bone sarcomas, also known as sarcomas of the skeletal system, can develop on the body’s bones and cartilage. Soft tissue sarcomas, on the other hand, occur in muscle, cartilage, fatty and connective tissue, and in the blood vessels.
Sarcomas affect the extremities in around half of all cases, of which around two-thirds are in the lower extremities such as the thighs, calves and feet. They also occur more frequently on the trunk of the body, for example on the chest wall or in the abdominal cavity. Around 9% of all sarcomas occur in the head and neck area.
How do sarcomas form?
Scientists do not yet know how bone sarcomas originate. However, there are certain risk factors that can lead to bone sarcomas:
- Radiation exposure
- Paget’s disease (a skeletal bone disorder)
- Genetic predisposition
The causes of soft tissue sarcomas are similarly unclear. However, a certain hereditary predisposition has also been shown in a very small number of soft tissue sarcomas. Some types of sarcoma also occur following contact with strong radiation, PVC or asbestos. Occasionally, certain viruses have also been found to be the cause. In the vast majority of sarcomas, however, the cause is unknown or unverifiable.
How many types of sarcoma are there?
The World Health Organisation (WHO) has divided sarcomas into over 150 different subtypes based on their tissue-specific characteristics. These subtypes differ considerably in terms of various criteria:
- Biological behaviour (How does the tumour develop, grow and behave?)
- Prognosis (What are the chances of recovery and life expectancy for people with the respective sarcoma?)
- Treatment response (How does the sarcoma react to certain treatment options?)
- Age incidence (How often does the sarcoma occur in certain age groups?)
As the types of sarcoma differ so widely and the number of subtypes is so enormous, precise identification is essential. This is the only way to develop a customised and effective tumour therapy – offering the best possible chances of recovery.
How often do sarcomas occur?
Sarcomas are comparatively rare, accounting for just 1% of all cancers. The Institute for Cancer Epidemiology recorded around 3,650 new cases in 2013. That is an average of around four new cases per 100,000 population.
The tumour occurs even less frequently in children, with around eleven out of every 1,000,000 under-fives diagnosed with this malignant carcinoma each year. In the 5-to-10 age group, the figure is as low as four per 1,000,000 children. With increasing age, the frequency then rises continuously. Sarcomas occur most frequently in 50 to 70-year-olds, with roughly equal incidence between women and men.

Contact us
The case management of WPE will assist you with questions you may have.
Phone: 0201 723 6600
Important Information
Benign growths in the soft tissue, which occur up to 100 times more frequently, do not count as sarcomas. Metastases in the bone, which occur in other primary tumors such as breast or prostate cancer, are also not sarcomas. They are all treated differently to genuine bone or soft tissue sarcomas.

Are you suffering from a sarcoma?
If you have been diagnosed with sarcoma and are now looking for a suitable therapy, please contact our Case Management team. Together we will clarify whether proton treatment is an option for you as a modern radiotherapy alternative.
Case Management: +49 (0) 201 723 6600
Treatment of sarcomas
Sarcomas are very rare diseases, and due to high differentiation into subtypes each respective sarcoma occurs even less frequently. As a result, standardisation is not always as possible as with other types of tumour.
That said, there are various therapy studies in which sarcoma patients are treated as a therapy aid. Many of these studies also take place in dialogue with international centres and organisations.
Where can sarcomas best be treated?
Treatment of malignant sarcomas should always be carried out in a specialist sarcoma centre. Given the many disciplines all working together, this is the best way to ensure the expertise to treat the tumour successfully.
At the Sarcoma Centre, experts in the respective disciplines then coordinate the treatment of the respective patients within what are known as Tumour Boards. A process that begins even before diagnosis and involves the following steps:
- Selection of the optimum sampling procedure (biopsy)
- Fine tissue examination (histology)
- Correct classification of the sarcoma
The team of experts also uses grading to determine what is referred to as the biological aggressiveness of the tumour. Staging is also used to determine the spread of the disease. Only when all these steps have been completed is the appropriate therapy selected – together with the patient.
How can sarcomas be treated?
Sarcoma treatment is always ‘multimodal’, i.e. different treatment methods such as surgery, chemotherapy and radiotherapy are mixed-and-matched to suit the classification and spread of the tumour. Soft tissue sarcomas, for example, are mostly removed surgically at the outset.
This is because some localised Grade I tumours can already be removed quite effectively – even completely – using this treatment. However, if complete removal is not possible, the sarcoma will remain under observation to start with.
With larger-spread tumours and with Grade II tumours and above, patients are often given chemotherapy or radiotherapy following surgery. This additional treatment is called adjuvant therapy and is intended to prevent a subsequent tumour relapse, or recurrence.
If, on the other hand, it is already clear in advance that complete removal of the sarcoma by surgical means is not possible, neoadjuvant therapy is used, i.e. radiotherapy and/or chemotherapy prior to surgery.
The aim of this is to shrink the tumour to a size that enables surgery to be successful. International experience shows that neoadjuvant radiotherapy is increasingly being favoured because radiation volumes can be limited more effectively and because post-operative functional capability is higher. However, this is also associated with more frequent complications such as wound healing disorders. Additional accompanying therapy measures are therefore often necessary.
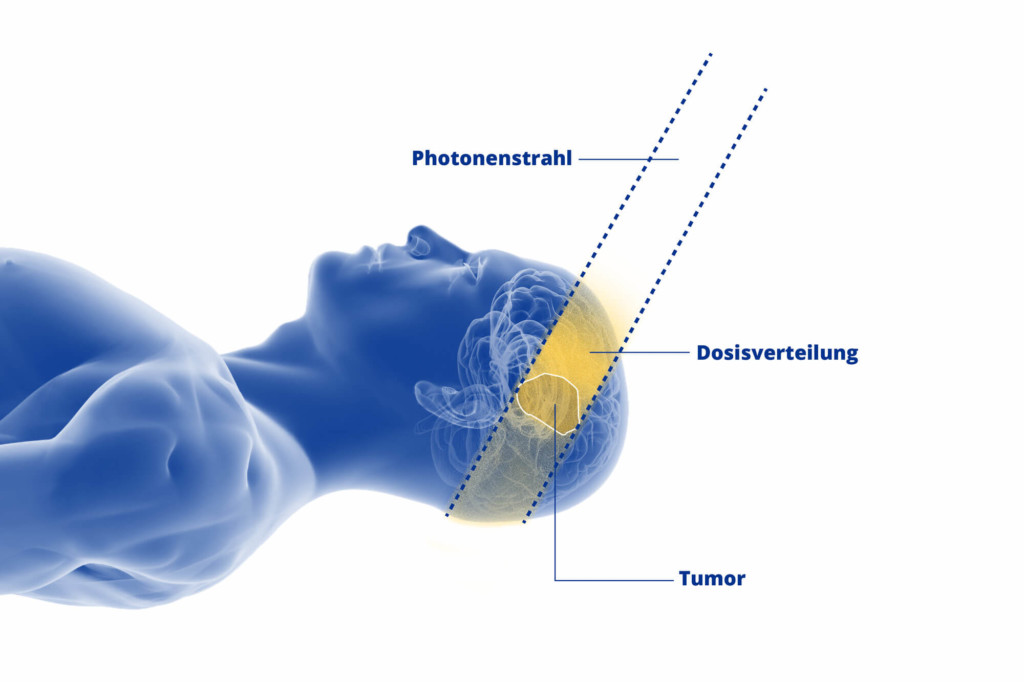
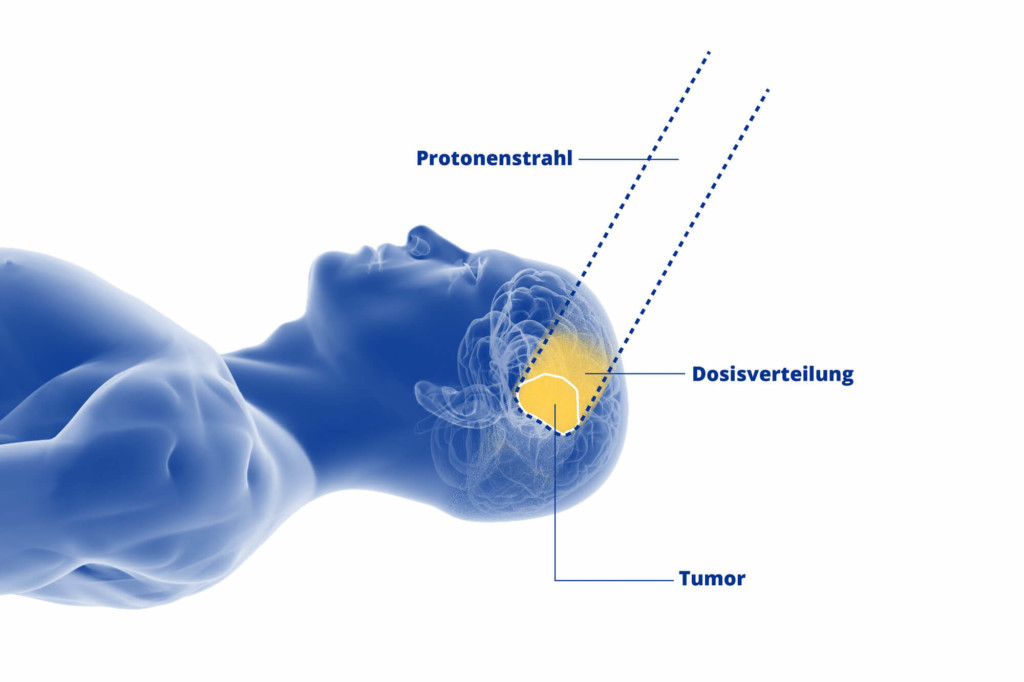
The advantage of proton radiotherapy is that it is as gentle as possible on healthy tissue. Protons emit very little radiation on their way to the tumour. They only release their maximum energy in the specified tumour zone and then come to an abrupt halt so that healthy cells behind the tumour are not irradiated.
This makes proton therapy an optimum treatment option especially for complex types of sarcoma where the soft tissue or bone tumour is surrounded by sensitive tissue. The ability to position the proton beams so precisely means the therapy team can also use higher doses of radiation, causing more damage to the tumour while at the same time sparing surrounding tissue. This increases both the quality of life and the life expectancy of sarcoma patients.
For which sarcomas does proton therapy aid the chances of recovery?
Essentially, proton radiotherapy can be used on all types of sarcoma. However, proton therapy is particularly suited to sarcomas that are inoperable or minimally operable. Sarcomas that are surrounded by extremely sensitive tissue also benefit from being treated with precisely targeted proton beams.
Here are some types of sarcoma for which proton therapy may offer improved chances of recovery or reduced side effects:
- Sarcomas of the base of the skull (chordomas and chondrosarcomas)
- Sarcomas of the facial bones (osteosarcomas)
- Sarcomas of the trunk of the body (soft tissue sarcomas)
Sarcomas of the spine (osteosarcomas)
Can proton therapy for sarcomas be combined with other therapies?
Essentially, proton therapy can easily be combined with other forms of treatment such as chemotherapy. However, the composition of the therapy always depends on various factors:
- Type of sarcoma (Which subtype is present?)
- Location of the sarcoma (Which organs are affected? What is the immediate environment of the tumour like?)
- Size of the sarcoma (Is surrounding tissue already affected? Or is the tumour too small for radiotherapy?)
To achieve the best possible treatment results, sarcomas are usually treated using several different forms of therapy which are specified by the interdisciplinary therapy team at regular Tumour Boards.
Sarcoma centre
There are specialized sarcoma centers in Germany. Try to find the relevant specialists in sarcoma treatment in your home country as well.

Rhabdomyosarcoma : the most common pediatric cancer in the group of soft tissue sarcomas
According to the guideline, soft tissue sarcomas are the fourth most common group of solid tumors in children – after tumors of the central nervous system (CNS), lymphomas and neuroblastomas. Within the group of soft tissue sarcomas themselves, rhabdomyosarcomas are the most common pediatric cancer:
More than 60 percent of all cases of rhabdomyosarcoma are diagnosed in children and adolescents; two thirds of them in children under the age of seven. Rhabdomyosarcomas develop in the tissue of the skeletal muscles. Depending on their location in the body, rhabdomyosarcomas manifest themselves with different symptoms.
Rhabdomyosarcomas are very suitable for irradiation with protons and are regularly treated in children at the WPE. If your child has a rhabdomyosarcoma, you are in the best hands with us. It is best to contact us right away.
Case Management: 0201 723 6600
Sarcoma proton therapy at WPE in the University Medical Centre of Essen
WPE (the West German Proton Therapy Centre Essen) is one of the leading centres for treating sarcomas with proton radiotherapy. As part of the University Medical Centre of Essen (a Sarcoma Centre certified by the German Cancer Society), we will work with all relevant specialist disciplines to determine the best possible treatment strategy for you. If you are already being treated at another sarcoma centre, proton therapy can still be carried out in Essen, and we will be happy to agree the treatment with your home hospital.
Who can be given proton therapy at WPE?
At WPE we use the most modern form of proton therapy: intensity-modulated ‘pencil beam scanning’ technology (PBS). This high-precision form of radiotherapy enables us to treat soft tissue sarcomas and bone sarcomas with high-dose radiation – with millimetre precision. As a patient, you benefit from the best possible chances of recovery, with side effects reduced as far as possible.
At WPE, we can irradiate the following sarcomas:
- Angiosarcoma
- Chondrosarcoma
- Chordoma
- Desmoid tumour / aggressive fibromatosis
- Dermatofibrosarcoma protuberans
- Endometrial stromal sarcoma
- Epithelioid sarcoma
- Ewing sarcoma / malignant peripheral neuroectodermal tumour (MPNET)
- Fibromyxoid sarcoma
- Clear cell sarcoma
- Leiomyosarcoma
- Liposarcoma
- Malignant peripheral nerve sheath tumour (MPNST)
- Osteosarcoma
- Pleomorphic sarcoma
- Rhabdoid tumour
- Rhabdomyosarcoma
- Solitary fibrous tumour
- Synovial sarcoma
How often are sarcomas treated with proton therapy at WPE?
Although sarcomas are rare, they are a frequently treated disorder at WPE. As a patient, you can therefore always rely on our comprehensive expertise – in childhood and adulthood disorders. We also have a wealth of experience in proton treatment for children.
Proton therapy shows its full potential especially in children who are still growing. This is because small children’s body tissue is particularly sensitive to radiation. For example, co-irradiation of bones can result directly in incorrect posture, curvature and inadequate bone growth. However, ultra-precise proton therapy and an experienced therapy team enable such complications to be avoided so that patients – whether adults or children – can subsequently have the best possible quality of life.
3,000 patients We treated our 3,000th tumour at the beginning of 2022. For us, this is both recognition and an incentive to keep pressing ahead.

4,000th Patient Treatment at WPE
In August 2023, the 4000th patient was treated at the WPE. She came from Romania and has a chordoma of the skull base. More information about her and her journey to Essen and during the therapy.
Treatment of infants under anesthesia
Patients must lie completely still during radiation treatment with protons. This is a major challenge, especially for small children. For a successful proton treatment, it may be necessary and sensible to sedate your child during the planning and actual therapy. Only anesthetists with the necessary experience in treating children with cancer perform this sedation at the WPE. Over 1000 children have already received their proton therapy at the WPE under light sedation.
What is the treatment process at WPE like?
If you are interested in WPE proton therapy for your sarcoma, you or your case doctor should start by sending us a therapy enquiry. Our Case Management team will receive your enquiry and be available to answer all your questions from then on. Any questions that Case Management cannot answer will be forwarded to our medical team.
Following the therapy enquiry, the procedure is as follows:
Once we are in possession of all the relevant information and documents, the doctors will decide whether proton radiotherapy is appropriate in your case, or will recommend any alternative treatment options. Individual enquiries are often discussed with colleagues from other relevant disciplines within the online Sarcoma Tumour Board – a panel of experts with specialist knowledge.
Once you have given your consent to proton radiotherapy, treatment commences. In most cases, the steps are as follows:
- Preparation of a made-to-measure positioning aid so that the sarcoma can be irradiated with precision during every radiotherapy session.
Use of imaging techniques, such as CT and, if necessary, MRI, so that our radio-oncological team and medical physicists can assess the exact location of the tumour and the surrounding organs.
Following planning and quality assurance, daily proton therapy is finally carried out after one to two weeks. These are usually outpatient sessions and take around six to eight weeks. Each individual radiotherapy session usually lasts no longer than half an hour, with actual proton radiotherapy taking just a few minutes.

WPE celebrates 10th anniversary
In September 2023 WPE celebrated 10 years of patient treatment at a festive and scientific meeting.
Important information for proton radiotherapy in combination with chemotherapy:
If combined radiotherapy and chemotherapy treatment is indicated for you or your child, it is possible to collaborate with the Sarcoma Centre at the University Medical Centre of Essen.
Cases involving sick children are also managed in close collaboration with the paediatric oncology department. This way we ensure treatment is simple and straightforward.
What information is required for the initial consultation?
If you are interested in proton radiotherapy for your sarcoma, we require the following documents from you for examination:
- Summarised medical report
- Any operation reports
- Up-to-date CT and MRI images
These can be submitted by you or your case doctor. Based on these documents, our radiation oncologists will then decide whether proton therapy is possible in your case. If so, we may need further documents at a later date for fine-tuning your treatment plan,
in which instance our Case Management team will inform you or your case doctors in good time so that your sarcoma treatment can commence promptly.
Please note that your enquiry can only be processed if the documents are complete and are presented in English or German.
What should be considered before treatment commences?
Proton therapy for sarcomas requires that there are no large metal implants in the area to be irradiated. These include things such as internal fixators used to keep parts of the vertebra stable.
If you have already undergone conventional radiotherapy, we will need to examine carefully the possibility of more radiotherapy involving protons. This is done taking into account your old radiotherapy records.
Overall, it is true to say that the treatment options and the course of your therapy at our centre always depend on the details of your specific medical condition. Factors such as fully-healed wounds and vision, hearing and kidney functions are additional key parameters which, depending on the location of the tumour, we take into account before initiating treatment.
Why undergo proton therapy at WPE?
The West German Proton Therapy Centre is one of the most advanced proton therapy centres in the world. Located in the heart of the Ruhr metropolitan area, we collaborate across disciplines and across the medical departments at the University Medical Centre of Essen to treat tumours whose locations call for the most precise radiotherapy possible.
We are particularly well positioned with regard to sarcomas. This is because we work closely with the certified Sarcoma Centre at the University Medical Centre of Essen. We also offer Europe’s largest programme of paediatric radiotherapy treatment.
Covering the cost of proton therapy
For us, treating patients from abroad is part of our daily work. Around 20% of our patients come from all over the world. We help all patients clarify the cost questions right from the start.
The most frequently asked questions on cost coverage are answered on a separate page.
Optimal therapy for rhabdomyosarcoma using genetic analysis
The rhabdomyosarcoma survival rate increases with optimal treatment. In order to determine the optimal cancer therapy in each case, it is essential to determine the exact type of tumor, ideally down to subtypes or special types. Based on their different tissue characteristics, a general distinction is made between alveolar rhabdomyosarcoma and embryonal rhabdomyosarcoma.
Contact our case management
Our Case Management staff will be pleased to advise you personally in all questions and control the therapy at the WPE.
In addition, they help you with the compilation of the required documentation and direct you to a radiotherapy specialist. Please contact us in the event that the sarcoma relevant for you is not listed here – we examine each individual case in detail
Case management
The case management of WPE will assist you with questions you may have
Phone: 0201 723 6600