
Proton therapy for brain tumours / CNS tumours at WPE
Everything you need to know.
Definition, frequency and development of CNS tumours
What are CNS tumours?
CNS tumours are tumours of the central nervous system (CNS). Almost 95% of them occur in the brain, but they can also develop in the brain stem or spinal cord. In addition, there are brain tumours that can form secondary tumours in the spinal cord, but where the primary tumour is the one in the brain.
In the following, we look primarily at the special requirements of brain tumours.
What types of CNS tumours are there?
There are a large number of different brain tumours, including both benign brain tumours and malignant brain tumours, all of which differ in terms of their characteristics, where they develop, and their prognosis and treatment. A distinction is also made between primary and secondary brain tumours:
- Primary brain tumours or tumours specific to the brain develop from cells of the brain tissue or the meninges.
- Secondary brain tumours are metastatic tumours of other tumour diseases that have settled in the brain.
The brain and our entire central nervous system consist of a wide variety of cells, each of which has its own tasks. The tumour type is determined by the location where the cancer cells occur and by the structures they affect. This is why there are many different types of CNS and brain tumours.
The following primary brain tumours exist:
- Gliomas: Originate in the brain support tissue (glial cells) of the CNS. Gliomas include (but are not limited to): astrocytomas, oligodendrogliomas, ependymomas and glioblastomas.
- Embryonic tumours: Originate in immature brain cells. This mainly affects children. The medulloblastoma falls into this category, the most common brain tumour in children.
- Meningioma: Develops from soft meninges.
- Neurinomas: Originate in cranial nerves or Schwan cells.
- CNS lymphoma: Caused by changes in the white blood cells (lymphocytes). CNS lymphoma belongs to the large group of malignant lymphomas that can occur anywhere in the body.
- Germ cell tumours: Originate in the germ cells. These include the germinoma and the chorionic carcinoma.
Brain tumour of the sella region: These tumours are located in the area of the bony base of the skull (sella turcica). These include the pituitary adenoma and the craniopharyngioma.
WHO classification of brain tumours
The World Health Organisation (WHO) categorises the severity of brain tumours into four different grades. Categorisation is based on the characteristics of the tumour tissue.
WHO Grade I corresponds to a slowly growing, benign tumour. WHO Grade IV, on the other hand, is usually a fast-growing, particularly malignant tumour.
Below is a list of CNS tumours in the four WHO grades:
- WHO Grade I: Pilocytic astrocytoma, neurinoma (acoustic neuroma), meningioma, pituitary adenoma/craniopharyngioma
- WHO Grade II: Diffuse astrocytoma, oligodendroglioma, ependymoma
- WHO Grade III: Anaplastic astrocytoma, anaplastic oligodendroglioma, anaplastic ependymoma
WHO Grade IV: Glioblastoma (Grade IV astrocytoma), medulloblastoma, primary malignant lymphoma, germinoma (primary germ cell tumour in the CNS)

Contact us
The case management of WPE will assist you with questions you may have.
Phone: 0201 723 6600
What are benign and malignant cancer cells?
Cancer cells are formerly normal cells whose DNA has changed and which are multiplying uncontrollably.
Malignant cancer cells can invade healthy cells and spread throughout the body via the blood, lymphatic or nervous system. Benign cancer cells, on the other hand, do not do this. Due to their local growth, however, they can displace healthy cells and trigger disorders, particularly in the head.
How frequently do CNS tumours occur?
Brain tumours are comparatively rare disorders. They account for only around 2% of all cancers in Germany.
The individual subtypes also vary greatly in their frequency and in age at onset. They occur particularly often between the ages of 50 and 70. CNS and brain tumours are rare in children. Nevertheless, they are the second most common type of cancer in children.

How do brain tumours develop?
Exact causes of brain tumours are only occasionally found. In most cases, no external triggers can be identified. However, the following reasons may be causes:
- Genetic predisposition
- Radioactive radiation
Contact with pesticides, herbicides, natural gas or crude oil
Can CNS tumours metastasise?
Brain tumours can spread to the spine, which is why this is often taken into account when treating the brain tumour. There are also numerous types of tumours whose metastatic tumours grow in the brain, such as breast or lung cancer.

Are you suffering from a brain tumour?
If you have a brain tumour and are looking for a suitable therapy, please contact our Case Management team.
Case Management: 0201 723 6600
Treatment of brain tumours
How can brain tumours be treated?
Various treatment methods can be used to treat brain tumours. These are used individually or in combination:
- Operation
- Chemotherapy
- Radiotherapy
- Immunotherapy (in certain instances)
The first step in determining the therapy is to determine the classification and grading of the tumour. To do this, a neuropathologist removes tumour tissue during a biopsy or operation and examines the cells in detail. An interdisciplinary tumour board then makes the specific treatment decision in conjunction with the patient.
Important information: For the best possible therapy, treatment should always take place in a special neuro-oncological centre as all the necessary specialist disciplines are represented there.
Surgery on brain tumours
Brain tumour surgery is used to reduce the size of the tumour or, in an optimum scenario, remove it completely. Brain tumour surgery also improves the conditions for subsequent treatments such as chemotherapy or radiotherapy.
Chemotherapy for brain tumours
Chemotherapy for brain tumours is used to kill the cancer cells or stop them from multiplying. It is systemic, i.e. it affects the entire body. Firstly, it can be carried out before the operation (neoadjuvant) in order to shrink the tumour in advance. Secondly, it can be carried out following surgical removal of the brain tumour (adjuvant) in order to kill off any remaining tumour cells.
Important information: Chemotherapeutic agents are not suitable for all types of brain cancer, as not all forms of brain tumour respond to chemotherapy.
Radiotherapy for brain tumours
Radiotherapy on brain tumours works locally and is used if the tumour cannot be removed with a sufficient margin of safety or is inoperable due to its location. Radiotherapy thus comes into its own with tumours in sensitive locations such as the head or craniospinal area which have a lot of sensitive tissue lying in close proximity. Radiotherapy for brain tumours often has to begin within a few weeks of surgery in order to prevent the tumour from growing again. In some cases, however, chemotherapy is also given in parallel with radiotherapy in order to increase the tumour cells’ sensitivity to radiation and thus maximise the impact of radiotherapy.

4,000th Patient Treatment at WPE
In August 2023, the 4000th patient was treated at the WPE. She came from Romania and has a chordoma of the skull base. More information about her and her journey to Essen and during the therapy.
Tumor irradiation in special cases
In the case of unfavorable tumor location or spread in the brain or spinal cord, local irradiation may not be sufficient. In such cases, it may be necessary to irradiate the entire cerebrospinal fluid system (corresponds to the entire head and spinal canal “craniospinal axis”).
Proton radiotherapy for brain tumours
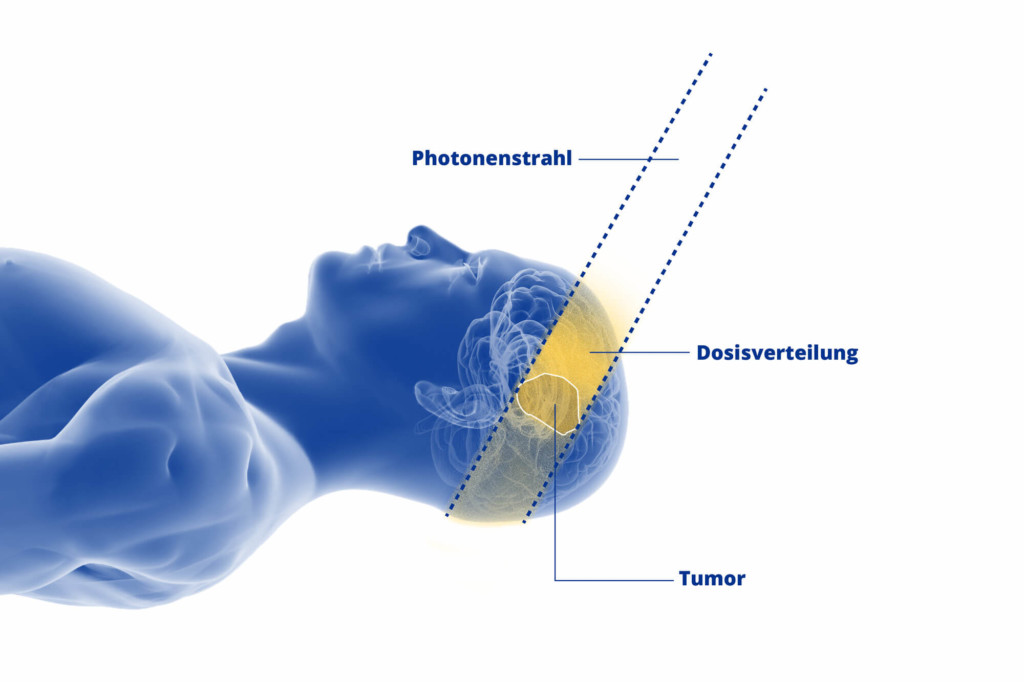
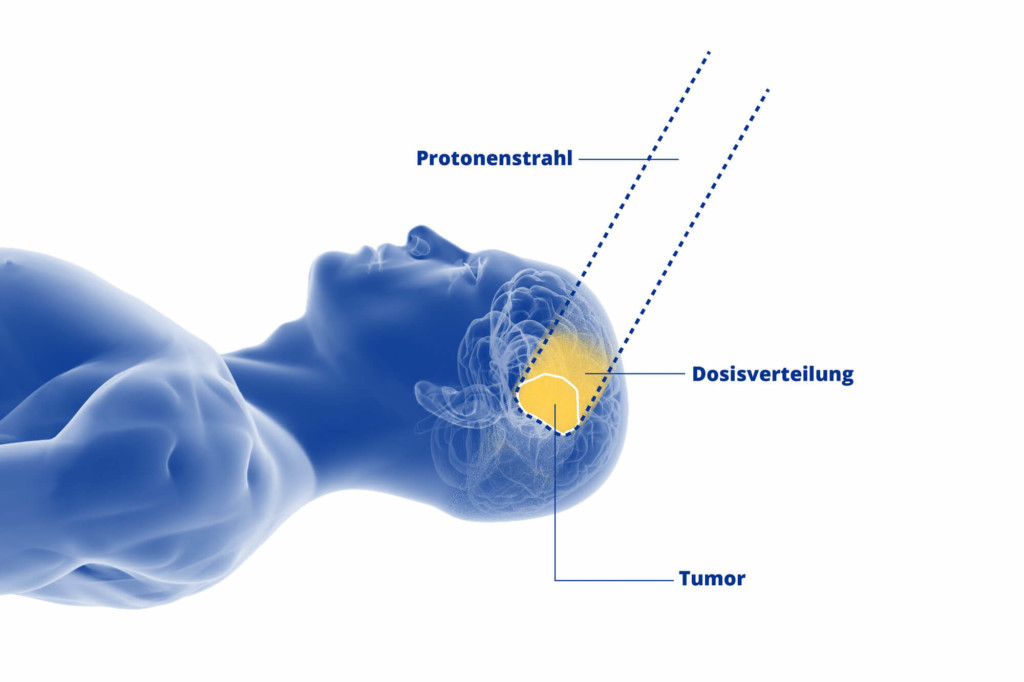
Proton irradiation is a modern and especially gentle type of radiotherapy for brain tumours. It also has one crucial advantage over conventional photon therapy: it can be directed at the diseased tissue with millimetre precision.
This is a great advantage, especially when irradiating CNS tumours, because radiation exposure of healthy tissue in and around the head and the base of the skull is reduced to an absolute minimum. The fact that the brain, spinal cord and parts of the body related to hearing and sight are exposed to little or no radiation reduces potential side effects. As well as increasing the chances of surviving a brain tumour, this can also improve patients’ long-term quality of life.
Can proton therapy be combined with other treatment methods?
In principle, proton therapy can be combined with other therapies. For example, it can be used post-operatively to destroy tumour cells that cannot be removed surgically. In certain cases, it is also used in conjunction with chemotherapy.
What side effects does proton therapy have when used on brain tumours?
During therapy, there may be occasional mild side effects due to the radiotherapy. This depends on what part of the body the beam enters.
For example, there may be varying degrees of reddening of the skin in the treated area. Hair loss can also occur when the proton beam hits the hair roots. Irritation of the mucous membranes in the mouth is also possible if the mouth is also irradiated. With advanced therapy, a feeling of fatigue may also occur as the body has to process the treatment.
Potential side effects from any parallel chemotherapy should also be taken into account. Potential case-by-case side effects during proton therapy are discussed in detail by the medical team during the information sessions.
Benefits of proton therapy
- Absolutely minimised radiation exposure for the surrounding organs that are still growing
- Lower side effects such as nausea, vomiting, pain, loss of appetite, etc.
- Reduced risk of secondary tumours
All of this hugely increases patients’ quality of life at the same time as ensuring higher acceptance during each individual radiotherapy session.
Proton therapy at WPE in the University Medical Centre of Essen
Why choose to be treated at WPE?
The West German Proton Therapy Centre is one of the most advanced proton therapy centres in the world. Located in the heart of the Ruhr metropolitan area, we treat tumours that require the most precise radiotherapy possible due to their location or the age of the patients. This is done in interdisciplinary collaboration with medical departments at the University Medical Centre of Essen and many external clinics.
We are particularly well positioned with regard to brain tumours – thanks to our close collaboration as part of the certified Neuro-oncology Centre at the University Medical Centre of Essen which has a broad range of expertise, even for difficult tumours. At WPE, we are particularly experienced in CNS tumours, in fact nearly 60% of the 3,000+ patients treated by us up to the beginning of 2022 fell into this category.
You can also rely on our expertise when it comes to treatment of children. We offer Europe’s largest programme of paediatric radiotherapy treatment.
Which CNS and brain tumours are treated at WPE?
At the West German Proton Therapy Centre Essen, we use the most advanced type of proton therapy – pencil beam scanning. This enables us to irradiate a large number of benign and malignant brain tumours with especially high precision.
We also have special expertise in treating rare tumours such as ependymomas, medulloblastomas, rhabdoid tumours, craniopharyngiomas and pituitary adenomas.
Indications for proton therapy include the following tumour types:
- AT/RT (atypical teratoid/rhabdoid tumour)
- Astrocytoma (also oligoastrocytoma, oligodendroglioma, etc.)
- Choroides plexus papilloma
- Ependymoma
- Grade I, II, III, IV glioma
- Glioblastoma
- Gliosarcoma
- Germ cell tumour (germinoma)
- Medulloblastoma, stPNET
- Meningioma
- Neuroblastoma
Examples of special tumour forms (some benign, some malignant):
- Acoustic neuroma
- Atypical neurocytoma
- Hemangiopericytoma
- Pituitary adenoma
- Craniopharyngioma
- Pilocytic astrocytoma
Also benign tumours in childhood (e.g. juvenile nasopharyngeal fibroma)

Recognition and motivation: The WPE treats its 3,000th patient.
Early 2022 WPE has treated its 3,000th patient – a benign brain tumour.
Treatment of ependymomas at the WPE
Ependymomas are among the tumors that are very frequently treated at the WPE. Almost 10 percent of all WPE patients to date have had an ependymoma.
Medulloblastoma
When planning treatment for medulloblastoma, there are no fixed age limits or fixed treatment plans. In addition to the profile of the tumor, the expert teams also take into account the individual preferences of the affected families.
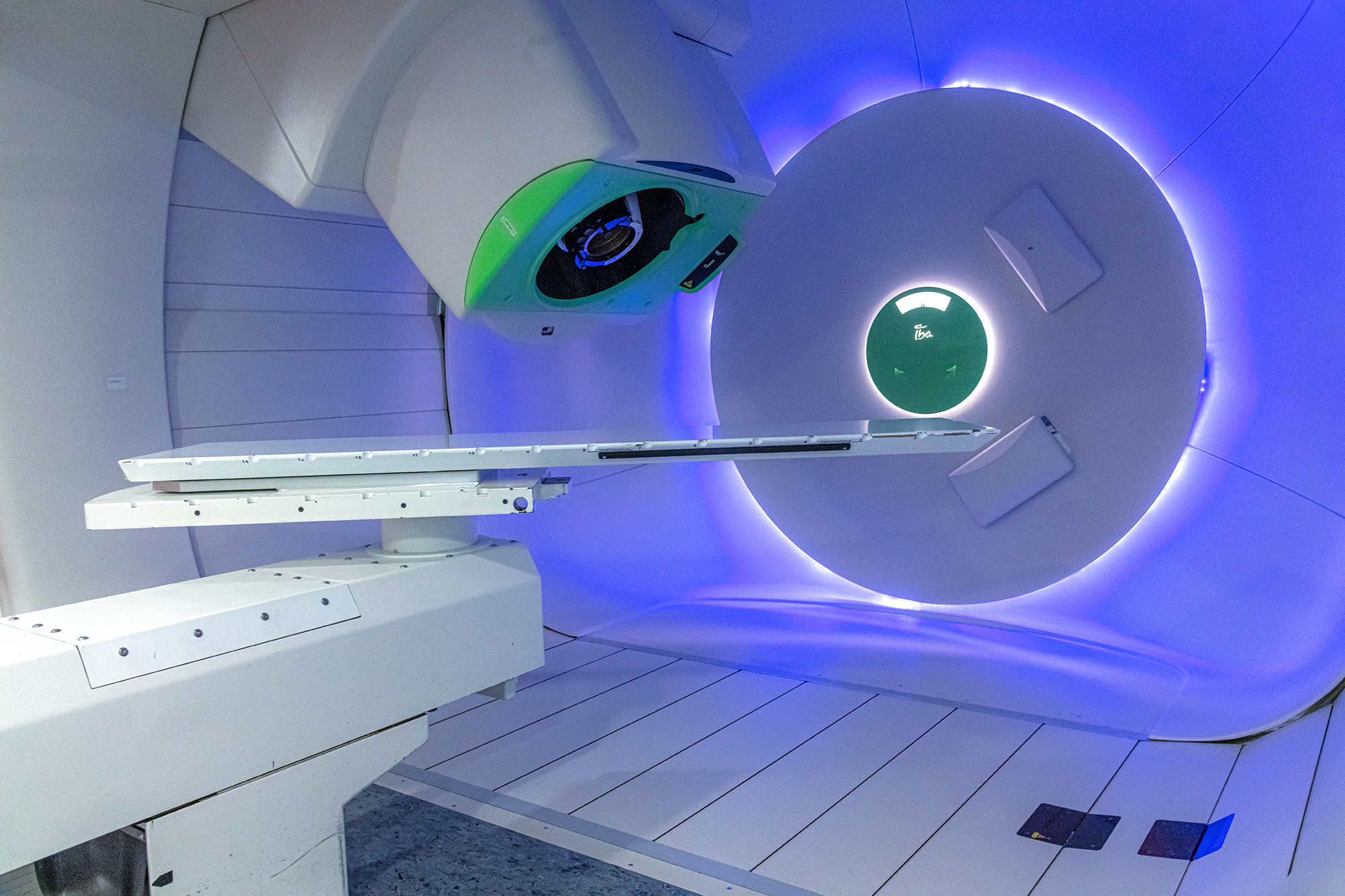
The strengths of proton therapy
Proton therapy can be especially effective on tumours whose location makes them difficult to operate on. For example, tumours at the base of the skull or on the brain stem are well suited to proton radiotherapy.
Precise irradiation means we can protect the pituitary gland (among other organs), preserving the body’s own hormone production.
What is the treatment process at WPE like?
If you are interested in proton therapy at WPE, you, your case doctor or family members should start by sending us a therapy enquiry. Our Case Management team will receive the enquiry and be available to answer all your questions from then on. Any questions that Case Management cannot answer will be forwarded to the case doctors.
Following the therapy enquiry, the procedure is as follows:
Once we are in possession of all the relevant information and documents, the doctors will decide whether proton radiotherapy is appropriate in your case, or will recommend any alternative treatment options. Individual enquiries are often discussed with colleagues from other relevant disciplines within the tumour board – a panel of experts with specialist knowledge.
If the team of experts decides to treat the brain tumour using proton therapy, treatment planning begins. For this purpose, we will invite you and a relative to an appointment at which we’ll explain the opportunities and risks of radiotherapy to you in detail.
Once you have given your consent to proton radiotherapy, treatment commences. It usually begins with the following steps:
- Preparation of a made-to-measure positioning aid so that the tumour can be irradiated with precision and in exactly the same way during every radiotherapy session.
- Use of imaging techniques, such as CT and, if necessary, MRI, so that our doctors and medical physicists can assess the exact location of the tumour and the surrounding organs. (If required, these examinations can be carried out under sedation, a short outpatient anaesthetic while breathing normally).
Following planning and quality assurance, daily proton therapy is finally carried out after one to two weeks. These are usually outpatient sessions and take place over a period of around four to seven weeks. Each individual radiotherapy session usually lasts no longer than half an hour, with actual proton radiotherapy taking just a few minutes.
Important information for proton radiotherapy in combination with chemotherapy:
If you are interested in proton radiotherapy for your CNS tumour, we require the following documents for examination:
- Summarised medical report
- Operation reports
- Up-to-date CT and MRI images
- Pathological findings
These can be submitted by you or your case doctor. Based on these documents, our radiation oncologists will then decide whether proton therapy is possible in your case. If so, we may need further documents at a later date for fine-tuning your treatment plan,
in which instance our Case Management team will inform you or your case doctors in good time so that your treatment can commence promptly. Please note that your enquiry can only be processed if the documents are complete and are presented in English or German.
What information is required for the initial consultation?
If you are interested in proton radiotherapy for your CNS tumour, we require the following documents for examination:
- Summarised medical report
- Operation reports
- Up-to-date CT and MRI images
- Pathological findings
These can be submitted by you or your case doctor. Based on these documents, our radiation oncologists will then decide whether proton therapy is possible in your case. If so, we may need further documents at a later date for fine-tuning your treatment plan,
in which instance our Case Management team will inform you or your case doctors in good time so that your treatment can commence promptly. Please note that your enquiry can only be processed if the documents are complete and are presented in English or German.
Cost coverage of proton therapy
The way in which the costs of proton therapy are covered varies depending on which country you come from.
We support all patients in clarifying costs right from the start.
Contact our case management
If you have questions or would like to know if proton therapy (PT) is an option for you, do not hesitate to contact us directly – even if your clinical picture is not listed here.
The course of therapy is always oriented to your individual indication and situation, advise you with the compilation of the required documentation, and initiate the examination of these by a radio-oncologist of the West German Proton Therapy Centre Essen (WPE).
Case management
The case management of WPE will assist you with questions you may have
Phone: 0201 723 6600